Abstract
Objective: This position paper reviews the potential prophylactic and therapeutic effects of photobiomodulation (PBM) on side effects of cancer therapy, including chemotherapy (CT), radiation therapy (RT), and hematopoietic stem cell transplantation (HSCT).
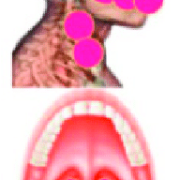
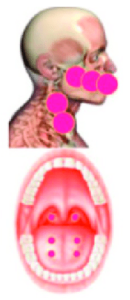
Background: There is a considerable body of evidence supporting the efficacy of PBM for preventing oral mucositis (OM) in patients undergoing RT for head and neck cancer (HNC), CT, or HSCT. This could enhance patients’ quality of life, adherence to the prescribed cancer therapy, and treatment outcomes while reducing the cost of cancer care.
Methods: A literature review on PBM effectiveness and dosimetry considerations for managing certain complications of cancer therapy were conducted. A systematic review was conducted when numerous randomized controlled trials were available. Results were presented and discussed at an international consensus meeting at the World Association of photobiomodulation Therapy (WALT) meeting in 2018 that included world expert oncologists, radiation oncologists, oral oncologists, and oral medicine professionals, physicists, engineers, and oncology researchers. The potential mechanism of action of PBM and evidence of PBM efficacy through reported outcomes for individual indications were assessed.
Results: There is a large body of evidence demonstrating the efficacy of PBM for preventing OM in certain cancer patient populations, as recently outlined by the Multinational Association for Supportive Care in Cancer/International Society of Oral Oncology (MASCC/ISOO). Building on these, the WALT group outlines evidence and prescribed PBM treatment parameters for prophylactic and therapeutic use in supportive care for radiodermatitis, dysphagia, xerostomia, dysgeusia, trismus, mucosal and bone necrosis, lymphedema, hand-foot syndrome, alopecia, oral and dermatologic chronic graft-versus host disease, voice/speech alterations, peripheral neuropathy, and late fibrosis amongst cancer survivors.
Conclusions: There is robust evidence for using PBM to prevent and treat a broad range of complications in cancer care. Specific clinical practice guidelines or evidence-based expert consensus recommendations are provided. These recommendations are aimed at improving the clinical utilization of PBM therapy in supportive cancer care and promoting research
in this field. It is anticipated these guidelines will be revised periodically.
Read more and access the PDF here. »