PBM successfully treating Covid-related Brain Fog
Robert Bowen and Praveen R. Arany
Shepherd University, West Virginia University, and University at Buffalo
March 28, 2023
Abstract:
There is increasing recognition of post-COVID-19 sequelae involving chronic fatigue and brain fog for which Photobiomodulation (PBM) therapy has been utilized. This open-label, pilot, human clinical study examined the efficacy of two PBM devices – e.g., a helmet (1070 nm) for transcranial (tPBM); and a light bed (660 and 850 nm) for whole body (wbPBM) over a four-week period, with 12 treatments for two separate groups (n = 7 per group). Subjects were evaluated with a neuropsychological test battery including Montreal Cognitive Assessment (MoCA), digit symbol substitution test (DSST), trail-making tests A and B, physical reaction time (PRT); and a quantitative electroencephalography system (WAVi), Pre- and Post- the treatment series. Each device for PBM delivery was associated with significant improvements in cognitive tests (p < 0.05 and beyond). Changes in WAVi supported the findings. This study outlines the benefits of utilizing PBM therapy (transcranial or whole-body) to help treat long COVID brain fog.
Non-Invasive Laser Light Therapy Could Improve Short-Term Memory by Up to 25 Percent
In a study published on December 2 in the journal Science Advances, laser light therapy has been shown to be effective in improving short-term memory.
Laser light therapy, which is non-invasive, could improve short-term, or working memory in people by up to 25 percent. This is according to new research demonstrated by scientists at the University of Birmingham in the UK and Beijing Normal University in China.
Transcranial Near Infrared Light Stimulations Improve Cognition in Patients with Dementia
Abstract
Dementia is a complex syndrome with various presentations depending on the underlying pathologies. Low emission of transcranial near-infrared (tNIR) light can reach human brain parenchyma and be beneficial to a number of neurological and neurodegenerative disorders. We hereby examined the safety and potential therapeutic benefits of tNIR light stimulations in the treatment of dementia. Patients of mild to moderate dementia were randomized into active and sham treatment groups at 2:1 ratio. Active treatment consisted of low power tNIR light stimulations with an active photobiomodulation for 6 min twice daily during 8 consequent weeks. Sham treatment consisted of same treatment routine with a sham device. Neuropsychological battery was obtained before and after treatment. Analysis of variance (ANOVA) was used to analyze outcomes. Sixty subjects were enrolled. Fifty-seven subjects completed the study and had not reported health or adverse side effects during or after the treatment. Three subjects dropped out from trial for health issues unrelated to use of tNIR light treatment. Treatment with active device resulted in improvements of cognitive functions and changes were: an average increase of MMSE by 4.8 points; Logical Memory Tests I and II by ~3.0 points; Trail Making Tests A and B by ~24%; Boston Naming Test by ~9%; improvement of both Auditory Verbal Learning Tests in all subtest categories and overall time of performance. Many patients reported improved sleep after ~7 days of treatment. Caregivers noted that patients had less anxiety, improved mood, energy, and positive daily routine after ~14-21 days of treatment. The tNIR light treatments demonstrated safety and positive cognitive improvements in patients with dementia. Developed treatment protocol can be conveniently used at home. This study suggests that additional dementia treatment trials are warranted with a focus on mitigating caregivers’ burden with tNIR light treatment of dementia patients.
Photobiomodulation with Near Infrared Light Helmet in a Pilot, Placebo Controlled Clinical Trial in Dementia Patients Testing Memory and Cognition
Abstract
Alzheimer’s disease (AD) is a common, chronic expensive debilitating neurodegenerative disease with no current treatments to prevent the physical deterioration of the brain and the consequent cognitive deficits. The current pathophysiology of Alzheimer’s disease is the accumulation of neurofibrillary tangles (NFTs) of hyperphosphorylated tau protein and amyloid-beta (Aβ) plaques. Antibody therapy of Tau and Amyloid beta, vaccines and other methods to decrease Tau and or Amyloid have not been successful after considerable pharmaceutical and biotech efforts. For example, Eli Lilly announced a major change to its closely watched clinical trial for the Alzheimer’s drug solanezumab which failed to reach statistical significance. Recently, a report on animal models using photomodulation with near infrared light to treat AD pathology in K369I tau transgenic model (K3) l engineered to develop neurofibrillary tangles, and the
APPs/PSEN1dE9 transgenic model (APP/PS1) to develop amyloid plaques. Mice were treated with NIR 20 times over a four-week period and NIR treatment (600-1000 nm) was associated with a reduction in the size and number of amyloid-β plaques in the neocortex and hippocampus. We now report a small pilot double blind, placebo-controlled trial (n=11) 6 active, 3 controls and 2 dropouts assessing the effect of 28 consecutive, six minute transcranial sessions of near infrared (NIR) stimulation using 1060-1080 nm light emitting diodes.
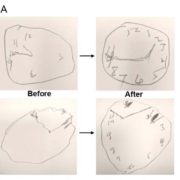
Subjects were independently diagnosed with dementia conducted in an outpatient behavioral healthcare clinic. IRB approval was obtained through the Quietmind Foundation’s institutional review Board (IRB). Results showed changes in executive functioning; clock drawing, immediate recall, praxis memory, visual attention and task switching (Trails A&B) as well as a trend of improved EEG amplitude and connectivity measures. Neuroplasticity has also been reported with NIR light stimulation and mitochondrial enhancement.
Preclinical Studies of Transcranial Photobiomodulation in the Neurological Diseases
Photobiomodulation (PBM) takes advantage of red and near-infrared light to induce therapeutic effects on various kinds of diseases, with transcranial PBM (tPBM) attracting most attention on neurological diseases. Displaying a noninvasive superiority over traditional treatment, tPBM is increasingly studied among research groups. Growing numbers of studies have been conducted in the last decade regarding neurological diseases; however, the research objects and lighting parameters among these papers varied from each other. This article introduces the biophotonics nature of PBM, records the experimental parameters of preclinical studies since 2014 and summarizes the application of tPBM on the neurobiological diseases in the past two decades. Under the summarized guidance of parameter setup, tPBM will be shining light in the prevention and treatment of neurological diseases.
Read more on Translational Biophotonics or download the PDF»
Effect of Near-Infrared Pulsed Light on the Human Brain Using Electroencephalography
In our previous study, the low-level laser (LLL) stimulation at the palm with a stimulation frequency of 10 Hz was able to induce significant brain activation in normal subjects. The electroencephalography (EEG) changes caused by the stimulation of light-emitting diode (LED) in normal subjects have not been investigated. This study aimed at identifying the effects of LED stimulation on the human brain using EEG analysis. Moreover, the dosage has been raised 4 times than that in the previous LLL study. The LED array stimulator (6 pcs LEDs, central wavelength 850 nm, output power 30 mW, and operating frequency 10 Hz) was used as the stimulation source. The LED stimulation was found to induce significant variation in alpha activity in the occipital, parietal, and temporal regions of the brain. Compared to the previous low-level laser study, LED has similar effects on EEG in alpha (8-12 Hz) activity. Theta (4-7 Hz) power significantly increased in the posterior head region of the brain. The effect lasted for at least 15 minutes after stimulation ceased. Conversely, beta (13-35 Hz) intensity in the right parietal area increased significantly, and a biphasic dose response has been observed in this study.
Read more on National Institutes of Health or download the PDF »
Experts review progress in using photobiomodulation therapy to treat diverse brain disorders
By Emily Henderson, B.Sc. |Newsmedical.com | October 14, 2021
Photobiomodulation (PBM) offers exciting opportunities for improving the life of patients with a diverse range of brain disorders. In this special collection of articles in the Journal of Alzheimer’s Disease experts review progress using PBM therapy to treat dementia, Alzheimer’s disease, Parkinson’s disease, and other disorders and suggest larger clinical trials should be conducted as soon as possible.
Transcranial photobiomodulation with 1064-nm laser modulates brain electroencephalogram rhythms
Abstract
Noninvasive transcranial photobiomodulation (tPBM) with a 1064-nm laser has been reported to improve human performance on cognitive tasks as well as locally upregulate cerebral oxygen metabolism and hemodynamics. However, it is unknown whether 1064-nm tPBM also modulates electrophysiology, and specifically neural oscillations, in the human brain. The hypothesis guiding our study is that applying 1064-nm tPBM of the right prefrontal cortex enhances neurophysiological rhythms at specific frequency bands in the human brain under resting conditions. To test this hypothesis, we recorded the 64-channel scalp electroencephalogram (EEG) before, during, and after the application of 11 min of 4-cm-diameter tPBM (CW 1064-nm laser with 162 mW / cm2 and 107 J / cm2) to the right forehead of human subjects (n = 20) using a within-subject, sham-controlled design. Time-resolved scalp topographies of EEG power at five frequency bands were computed to examine the tPBM-induced EEG power changes across the scalp. The results show time-dependent, significant increases of EEG spectral powers at the alpha (8 to 13 Hz) and beta (13 to 30 Hz) bands at broad scalp regions, exhibiting a front-to-back pattern. The findings provide the first sham-controlled topographic mapping that tPBM increases the strength of electrophysiological oscillations (alpha and beta bands) while also shedding light on the mechanisms of tPBM in the human brain.
Effects of Home Photobiomodulation Treatments on Cognitive & Behavioral Function, Cerebral Perfusion and Resting-State Functional Connectivity in Patients with Dementia
This study sought to replicate and build upon a previously published cases series report describing improved cognitive function in five patients with mild to moderate dementia after 12 weeks of transcranial and intranasal near-infrared (NIR) PBM therapy.
In collaboration with the University of California San Francisco using the Neuro Gamma device on neural connectivity and cerebral blood flow.