The Emerging Role of Photobiomodulation in COVID-19 Therapy Part II
The Emerging Role of Photobiomodulation in COVID-19 Therapy Part II Whole Organ PBM Case Studies for Acute & Long COVID (European Society of Medicine)
Purpose: To empirically confirm the utility of photobiomodulation (PBM) in the treatment of acute and long COVID-19 guided by a mechanistic analysis of the photochemical effects of pulsed light on SARS-CoV-2 infections and disease progression.
PBM successfully treating Covid-related Brain Fog
Robert Bowen and Praveen R. Arany
Shepherd University, West Virginia University, and University at Buffalo
March 28, 2023
Abstract:
There is increasing recognition of post-COVID-19 sequelae involving chronic fatigue and brain fog for which Photobiomodulation (PBM) therapy has been utilized. This open-label, pilot, human clinical study examined the efficacy of two PBM devices – e.g., a helmet (1070 nm) for transcranial (tPBM); and a light bed (660 and 850 nm) for whole body (wbPBM) over a four-week period, with 12 treatments for two separate groups (n = 7 per group). Subjects were evaluated with a neuropsychological test battery including Montreal Cognitive Assessment (MoCA), digit symbol substitution test (DSST), trail-making tests A and B, physical reaction time (PRT); and a quantitative electroencephalography system (WAVi), Pre- and Post- the treatment series. Each device for PBM delivery was associated with significant improvements in cognitive tests (p < 0.05 and beyond). Changes in WAVi supported the findings. This study outlines the benefits of utilizing PBM therapy (transcranial or whole-body) to help treat long COVID brain fog.
Near Infrared Light (940nm) Improves COVID Outcomes: Exciting Randomized Control Trial
Roger Seheult, MD of MedCram examines an exciting randomized control trial demonstrating the effects of near infrared light on COVID-19.
See all Dr. Seheult’s videos here.
Light as a Cure in COVID-19: A Challenge for Medicine
Abstract
Light and lasers, as high-tech devices whose medical potential has yet to be fully discovered, have made important contributions to medicine, even in the current pandemic. The main aim of this review was to investigate how light was applied as a therapeutic tool during a crisis triggered by COVID-19. Another goal was to encourage scientists and industry to quickly design new at-home photobiomodulation therapy (PBMT) and/or antimicrobial photodynamic therapy (aPDT) easy to use systems to end this pandemic, especially for those who believe in high-tech but would never get vaccinated. This review revealed that PBMT has been successfully applied as adjunct therapy, in combination with conventional medical treatment, and as a pioneering action in SARS-CoV-2 infection, demonstrating significant improvements in airway inflammation and general clinical condition of patients, a faster recovery, avoiding intensive care unit (ICU) hospitalization, mechanical ventilation, mortality, and overcoming long-term sequelae. Application in only a limited number of cases strongly suggests the need for future randomized, placebo-controlled clinical trials to objectively determine the action and effects of PBMT in COVID-19. Implementation of unparalleled theragnostics methods and light-based techniques for disinfection of spaces, air, skin, mucosae, and textures to decrease the load of SARS-CoV-2 virus would save lives, time, and money. In this ongoing and challenging search for the seemingly intangible end of this pandemic, a non-invasive, easily accessible, safe, and side-effect-free adjuvant method appears to be PBMT, alone or in synergistic combination with aPDT, which has been shown to work in COVID-19 and opens unprecedented potential for use as home self-treatment to end the pandemic.
Rationale for 1068 nm photobiomodulation therapy (PBMT) as 2 a novel, non-invasive treatment for COVID-19: roles of NO and 3 Hsp70
Abstract
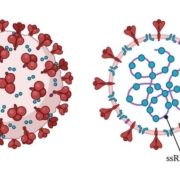
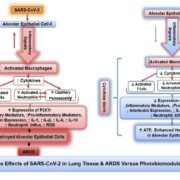
Researchers from across the world are seeking to develop effective treatments for the ongoing coronavirus disease 2019 (COVID-19) outbreak, which arose as a major public health issue in 9 2019, and was declared a pandemic in early 2020. The pro-inflammatory cytokine storm, acute respiratory distress syndrome (ARDS), multiple-organ failure, neurological problems, and thrombosis 11 have all been linked to severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) fatalities. 12 The purpose of this review is to explore the rationale for using photobiomodulation therapy (PBMT) 13 of the particular wavelength 1068 nm as a therapy for COVID-19, investigating the cellular and 14 molecular mechanisms involved. Our findings illustrate the efficacy of PBMT 1068 nm, through 15 cytoprotection, nitric oxide (NO) release, inflammation changes, improved blood flow and regulation in heat shock proteins (Hsp70). We propose, therefore, that PBMT 1068 is a potential effective 17 and innovative approach for avoiding severe and critical illness in COVID-19 patients, although 18 further clinical evidence is required.
Therapeutic Application of Light and Electromagnetic Fields to Reduce Hyper-Inflammation Triggered by COVID-19
Abstract
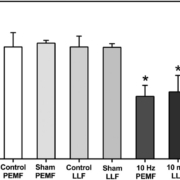
COVID-19 – related morbidity is associated with exaggerated inflammation and cytokine production in the lungs, leading to acute respiratory failure. The cellular mechanisms underlying these so-called ‘cytokine storms’ are regulated through the Toll-like receptor 4 (TLR4) signaling pathway and by ROS (Reactive Oxygen Species). Both light (Photobiomodulation) and magnetic fields (e.g., Pulsed Electro Magnetic Field) stimulation are noninvasive therapies known to confer anti-inflammatory effects and regulate ROS signaling pathways. Here we show that daily exposure to two 10-minute intervals of moderate intensity infra-red light significantly lowered the inflammatory response induced via the TLR4 receptor signaling pathway in human cell cultures. Anti-inflammatory effects were likewise achieved by electromagnetic field exposure of cells to daily 10-minute intervals of either Pulsed Electromagnetic Fields (PEMF), or to Low-Level static magnetic fields. Because current illumination and electromagnetic field therapies have no known side effects, and are already approved for some medical uses, we have here developed protocols for verification in clinical trials of COVID-19 infection. These treatments are affordable, simple to implement, and may help to resolve the acute respiratory distress of COVID-19 patients both in the home and in the hospital.
Whole-Organ Transdermal Photobiomodulation (PBM) of COVID-19: A 50-Patient Case Study
Abstract
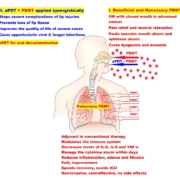
A non-randomized 50-person case study of COVID-19 positive patients was conducted employing (for the first time) a regimen of whole-organ deep-tissue transdermal dynamic photobiomodulation (PBM) as a primary (or exclusive) therapeutic modality in the treatment of coronavirus. Therapy sessions comprised algorithmically alternating red (650 nm) and near infrared (850 nm) LEDs with average irradiance of 11 mW/cm2 dynamically sequenced at multiple pulse frequencies. Delivered via 3-D bendable polymeric pads maintaining orthogonal optical incidence to body contours over 1,000 cm2, a single 84-min session concurrently delivered 20 kJ to the sinuses and 15 kJ to each lung at skin temperatures below 42 ◦C. Therapeutic outcomes observed include significant reductions in the duration and severity of disease symptoms. Acute conditions including fever, body aches, and respiratory distress comprising paroxysmal coughing; lung congestion, dyspnea and hypoxia; sinus congestion; acute eye inflammation; and extreme malaise were eliminated in 41/50 patients within 4-days of commencing PBM treatments with 50/50 patients fully recovering within three-weeks with no supplemental oxygen requirements. SpO2 concentrations improved as much as 9 points (average 2.5 points) across the entire study population. The PBM sessions required to completely resolve COVID-19 conditions appears mono- tonically correlated to the time-to-treatment (TTTx) — the delay between the onset of a patient’s symptoms and commencing PBM therapy. In contrast, acute inflammatory symptoms were resolved within 4-days irrespective of TTTx.
Evaluation of Adjunctive Photobiomodulation (PBMT) for COVID-19 Pneumonia via Clinical Status and Pulmonary Severity Indices in a Preliminary Trial
Introduction: The COVID-19 pandemic spread rapidly throughout the world, causing millions of infections, hundreds of thousands of deaths, and overloaded hospitals and intensive care units, with patients in need of critical care management. The initial hallmarks of COVID-19 were cytokine storm and acute respiratory distress syndrome (ARDS). Some patients are asymptomatic and recover spontaneously while others experience progressive symptoms leading to mild, moderate, or serious cases. Many serious cases require admission to intensive care units (ICUs) and ventilation support. The exceptional number of patients who died while receiving optimal medical care and ventilator support remains an enigma and successful treatment strategies remain to be found.
Case and outcomes: During the period from March 2020 to May 2020, we performed a preliminary clinical trial with a parallel design for the evaluation of PBMT on COVID-19 pneumonia (ClinicalTrials.gov identifier: NCT04391712). Before obtaining Institutional Review Board (IRB) approval, the US Food and Drug Administration assessed the MLS scanner-equipped laser and deemed it was a nonsignificant risk device. Subsequently, the IRB, and the Clinical Research Review Committee of the Lowell General Hospital (Massachusetts, USA) approved the clinical protocol for PBMT treatment of COVID-19 pneumonia. All patients provided written informed consent for participation in this trial. A preliminary 10 patient study was approved by the hospital. Patients were assigned to the PBMT group (standard medical care plus adjunctive PBMT) or control group (standard medical care) using the Sealed Envelope computer application (Table 1). There was no masking of the treatment group, and the study was performed in an open-label fashion. Inclusion criteria were: SARS-CoV-2 infection confirmed by nasopharyngeal swab and RT-PCR on an Abbott ID system upon hospitalization, age 18–90 years, and pulmonary compromise requiring oxygen support. Patients had to be able to self-prone or support themselves in a self-sitting position to facilitate the administration of PBMT. Exclusion criteria included patients who required ventilator management, those with autoimmune disorders or inflammatory conditions not related to COVID-19, and pregnancy. The trial was conducted in accordance with the Declaration of Helsinki.
Conclusion: This study demonstrates the potential benefits of adjunctive PBMT in COVID-19 pneumonia. The use of PBMT in the early stages of severe ARDS in COVID-19 patients may improve pulmonary and clinical status and reduce the need for ventilator support and ICU stay. Adjunctive PBMT may decrease hospital stay and enhance the recovery process. Clinical status improvement was supported by an increase in SpO2 during the treatment sessions, the rapid relief of respiratory symptoms, and improved CXR findings. There was no incidence of mortality or major reported side effects in the PBMT group. The mortality rate was 40% in the control group and 40% of patients continue to experience pulmonary sequelae. The patients in the PBMT group recovered without needing ICU admission or mechanical ventilation. Conversely, 60% of patients in the control group required ICU admission and ventilation. Clinical trials with larger group sizes are necessary to confirm the effects of PBMT on COVID-19 pneumonia